'It's incredible, like science fiction': How a new wave of immunotherapy is eliminating cancers
 Emmanuel Lafont/ BBC
Emmanuel Lafont/ BBCAfter nearly 100 years of development, treatments that bolster the body's immune system to fight cancer are coming of age – and saving patients' lives.
When 71-year-old Maureen Sideris was treated for colon cancer in 2008, she had to go under the knife. Her treatment was successful, but the post-operative recovery process was gruelling.
Fourteen years later, Sideris, who lives in New York, was diagnosed with oesophageal cancer – and this time, her treatment, offered through a clinical trial, looked radically different. Every three weeks, she travelled to Memorial Sloan Kettering Cancer Center in New York City for 45 minute-long infusions of a drug called dostarlimab.
After just four months of treatment, Sideris' tumour had disappeared – without surgery, chemotherapy or radiation, and with her only major side effect being adrenal insufficiency that causes fatigue. "It's unbelievable," she says. "It's almost like science fiction."
And yet, it's real. Sideris is one of a growing number of patients to benefit from immunotherapy for cancer, a treatment method hitting its stride after more than a century of development.
"I get choked up and have goosebumps," says Jennifer Wargo, a professor of surgical oncology and an immunotherapy researcher at MD Anderson Cancer Center in Texas. "People are living, and living with good quality lives. We're talking about cures."
The body has a natural ability to "detect and eliminate cells that look like not-you," explains Karen Knudsen, chief executive of the Parker Institute for Cancer Immunotherapy, a US nonprofit that furthers immunotherapy development. If all is working well, that should include cells that have become cancerous. But sometimes, cancer cells evade or outsmart that system, leading to dangerous unchecked growth. They hide, in plain sight, indistinguishable from the healthy cells around them.
Immunotherapy's goal is to unmask those cancer cells so the immune system can see them for what they are. It bolsters the immune system's defences so it can locate and destroy cancerous cells – with potentially incredible results.
How immunotherapy fights cancer today
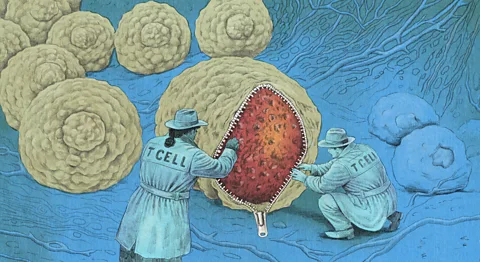
Two of the best-known forms of immunotherapy are CAR T-cell therapies and immune checkpoint inhibitors. CAR T-cell therapies involve extracting T cells (the highly specific immune cells that hunt down and kill off particular foreign invaders) from a patient's blood, modifying them in a lab so they can find and attack cancer cells and then letting the souped-up T cells loose in the body. These therapies are currently used to treat blood cancers.
Immune checkpoint inhibitors, meanwhile, are drugs that disable a built-in "off" switch in the immune system. This safeguard has an important purpose – it prevents overly aggressive immune responses that damage healthy cells. Some cancer cells can flip the off switch, however, causing the T cells to stand down so they escape detection. Immune checkpoint inhibitors prevent that from happening, meaning that the T cells identify the cancer cells as a threat and launch an assault. The scientists who pioneered this innovation won a Nobel Prize in 2018, and the drugs are today used across many cancer classes.
Still, both methods have limitations. Although research is ongoing, scientists have struggled to make CAR T-cell therapies work against solid tumours (as opposed to blood cancers), which account for more than 90% of new diagnoses. The treatment is also expensive and labour-intensive to administer.
 Emmanuel Lafont/ BBC
Emmanuel Lafont/ BBCImmune checkpoint inhibitors, meanwhile, can come with a "kaleidoscope of side effects," says Samra Turajlic, a medical oncologist at the Francis Crick Institute in London. That is because the immune system's off-switches are meant to prevent the body from attacking its own tissues and removing that defence may therefore endanger non-cancerous cells as well as tumours. According to the US National Cancer Institute, common side effects include skin rashes, diarrhoea and fatigue, while in rare cases it can cause inflammation of the liver, heart and kidneys.
That trade-off may be worth it, if the drug controls an aggressive cancer. But it doesn't always work that way. A major problem facing the entire oncology field, Turajlic says, is that no immunotherapy works in 100% of recipients. There are many potential reasons, ranging from the structure of the tumour, which can reduce its accessibility to the immune system, to the characteristics of immune cells themselves.
In general, somewhere between 20% and 40% of patients respond to immunotherapy. That means a lot of patients – the majority, in fact – are opening themselves up to side effects, not to mention wasted time and hope, without much upside.
Multipronged approaches
How can more patients benefit from immunotherapy? Researchers are attacking that problem from lots of different angles.
Wargo's research, while preliminary, suggests that patients who follow high-fibre diets may see better results through changes to the gut microbiome that may affect both the immune system and the tumour. Other surprising research indicates that statins, inexpensive and accessible cholesterol-lowering drugs, may enhance the effects of immunotherapy, through unexpected changes to cell communication. Even the timing of treatment may matter, with some recent research hinting that patients dosed early in the day fare better than those treated later.
Combining immunotherapy with other cancer treatments, such as radiation or ultrasound, may be another way to boost response rates. "Radiation can actually…make the tumour visible to the immune system," explains Sandra Demaria, at the Weill Cornell Medical Center who has researched this combined approach. Ultrasound therapy, which harnesses high-frequency sound waves to attack tumours, may do the same.
Other researchers are taking advantage of immunotherapy's capacity for customisation and carefully matching patients to their best possible treatment.
Personalised medicine is generating excitement in many disciplines, but Knudsen emphasises that it is particularly important for oncology, given the heterogeneity of the disease. "Cancer is not one disease," Knudsen says. "It's 200 different diseases, and they all arise due to different reasons and they have to be treated differently." Even two patients with the exact same type and stage of cancer may have different diseases at a cellular level.
"The field is at an inflection point," Demaria says. "We can now move toward treating not the cancer, but actually the patient."
Scientists at Memorial Sloan Kettering Cancer Center have already trialled one promising strategy, based on the finding that tumours with a particular genetic profile tend to respond well to immune checkpoint inhibitors such as dostarlimab. In two small trials from 2022 and 2024 treating rectal cancers with this profile, the treatment completely eradicated tumours. The team then expanded their research to include 117 patients with various types of tumours – including oesophageal, bladder and stomach – that carried the same genetic signature. Out of 103 people who finished the full course of treatment, 84, including Sideris, saw complete disappearance of their tumours, with only two requiring additional surgery.
Researchers from MD Anderson have reported similar results for an approach using a different checkpoint inhibitor. And other groups have shown that – even if patients do undergo surgery eventually – their operative results may be better, in at least some cases, if the tumours are first attacked with immunotherapy.
While more research is needed, such findings are promising because they open the door to a less invasive yet highly effective era of treatment, says Luis Diaz, head of solid tumour oncology at Memorial Sloan Kettering Cancer Center. "We have to move from Medieval times to modern times," he says. "To remove your rectum or your stomach or bladder – we've got to do better than that."
The caveat is that only around 5% of tumours have the genetic makeup that makes them a good fit for the surgery-free immunotherapy treatment Diaz and his colleagues studied. "The other 95% need something as good," he says.
The promise of cancer vaccines
To that end, researchers continue to look for new immunotherapy approaches and try to improve upon older ones – such as cancer vaccines.
Traditional vaccines introduce the body to parts of a pathogen, such as a virus, so it can practice mounting an immune response to the real thing. A similar concept could work in cancer, Knudsen says – except it could be used to treat the illness rather than prevent it.
 Emmanuel Lafont/ BBC
Emmanuel Lafont/ BBCCancer cells are adorned with various surface proteins. Using vaccine technology, researchers may be able to train a patient's immune system to recognise and target these proteins, triggering a robust response against their specific cancer, Knudsen explains.
There's already some preliminary evidence to support this approach. Researchers from Dana-Farber Cancer Institute in the US recently created personalised vaccines for nine people with a type of kidney cancer. After their tumours were surgically removed, the patients were vaccinated to rid their bodies of any lingering tumour cells.
In research published in 2025, the team reported that all nine patients launched a targeted anti-cancer immune response and remained cancer-free years after surgery. Personalised vaccines have also shown promise for treating melanoma.
"It's a bold new world out there," Knudsen says. "It's the definition of precision medicine. We can now perhaps, in a very quick way, develop vaccination strategies against the exact tumour you have."
Despite this excitement, the road ahead is long.
More studies are needed to back up some of the encouraging methods under investigation, and to reach a future in which doctors can precisely and reliably match patients with treatments that will work against their specific cancers. "There's been a lot of very promising targets and new agents that did not progress beyond early-phase clinical trials," cautions Demaria.
It is possible that a subset of patients won't respond to any kind of immunotherapy, Diaz says. Cancers have different "superpowers" that allow them to grow and thrive, he says, and the immune system is a better opponent for some than others.
But for patients who do respond, immunotherapy is already proving both lifesaving and life-changing.
Sideris, the New York patient who took part in Diaz's trial, feels like part of a brighter future for oncology. "We're going in such a great direction," she says. "One of the doctors [told me] that within 10 years time, doing any kind of chemo and radiation is going to be like bloodletting – so old-fashioned."
--
If you liked this story, sign up for The Essential List newsletter – a handpicked selection of features, videos and can't-miss news, delivered to your inbox twice a week.
For more science, technology, environment and health stories from the BBC, follow us on Facebook and Instagram.
